Is oculoplastic surgery covered by insurance? Navigating the complexities of insurance coverage for this specialized eye surgery can be tricky. Different procedures, insurance plans, and pre-authorization requirements all play a role in determining whether your care will be fully or partially covered. Understanding the factors that influence coverage is key to planning and managing your potential costs.
This guide delves into the ins and outs of oculoplastic surgery insurance coverage, exploring various scenarios, potential costs, and steps to take before and after your procedure. We’ll cover everything from common procedures and their likelihood of coverage to the necessary pre-authorization processes and documentation required. Plus, we’ll equip you with resources to help you navigate the process and understand your financial responsibilities.
Overview of Oculoplastic Surgery
Oculoplastic surgery is a specialized branch of ophthalmology focused on the structures surrounding the eye. It’s a delicate and intricate field, demanding a deep understanding of facial anatomy and meticulous surgical technique. This specialized care often involves intricate procedures to correct a wide range of conditions impacting the eyelids, tear ducts, orbital bones, and surrounding tissues.Oculoplastic surgery encompasses a spectrum of procedures, each tailored to address specific eye-related concerns.
From correcting droopy eyelids to restoring proper tear drainage, these procedures can significantly improve patients’ quality of life. The procedures vary greatly in complexity, from relatively straightforward techniques to more intricate ones, each with its own set of potential complications and benefits.
Types of Oculoplastic Procedures
Oculoplastic surgery encompasses a range of procedures aimed at restoring or improving the function and appearance of the structures around the eye. These procedures address a variety of issues, from cosmetic concerns to correcting functional problems.
- Blepharoplasty: This procedure involves reshaping the eyelids to address excess skin, fat, or muscle. Common reasons include drooping eyelids (ptosis), bags under the eyes (periorbital fat), or sagging skin around the eyelids. The outcomes of blepharoplasty can include a more youthful and refreshed appearance, improved vision, and a reduction in the discomfort associated with excess skin and fat.
- Orbital Decompression Surgery: This procedure aims to increase the size of the eye socket (orbit) to alleviate pressure on the optic nerve and eye muscles, often in cases of orbital tumors or conditions like Graves’ disease. Success rates vary depending on the underlying cause, but the potential benefits include improved vision and reduced pain.
- Dacryocystorhinostomy (DCR): This procedure redirects blocked tear ducts, allowing tears to drain properly. This surgery can address chronic tearing, dry eyes, and infections. Outcomes often involve improved tear drainage and a reduction in discomfort associated with chronic tearing.
- Orbital Tumors and Trauma Repair: Oculoplastic surgeons play a crucial role in addressing and repairing conditions like orbital tumors, fractures of the eye socket, and other traumatic injuries. This involves careful assessment and precise surgical intervention to restore the delicate anatomy of the eye socket and surrounding structures. Outcomes are highly variable, depending on the extent and severity of the damage.
Conditions Addressed by Oculoplastic Surgery
A wide range of conditions can benefit from oculoplastic surgery. These procedures address both functional and cosmetic concerns related to the delicate structures around the eye.
- Eyelid Disorders: Conditions like ptosis (drooping eyelids), entropion (inward turning of the eyelid), ectropion (outward turning of the eyelid), and chalazion (a cyst on the eyelid).
- Orbital Disorders: Conditions such as Graves’ ophthalmopathy, orbital tumors, and orbital fractures.
- Tear Duct Problems: Conditions like dacryoadenitis (inflammation of the tear gland), punctal stenosis (narrowing of the tear duct opening), and nasolacrimal duct obstruction.
Comparison of Oculoplastic Procedures
| Procedure | Common Uses | Typical Outcomes |
|---|---|---|
| Blepharoplasty | Drooping eyelids, bags under eyes, sagging skin | Youthful appearance, improved vision, reduced discomfort |
| Orbital Decompression | Increased orbital pressure, Graves’ ophthalmopathy | Improved vision, reduced pain, reduced pressure |
| Dacryocystorhinostomy | Blocked tear ducts, chronic tearing | Improved tear drainage, reduced discomfort |
| Orbital Tumor/Trauma Repair | Tumors, fractures, injuries | Restoration of orbital structure, improved vision/function |
Insurance Coverage Factors for Oculoplastic Surgery
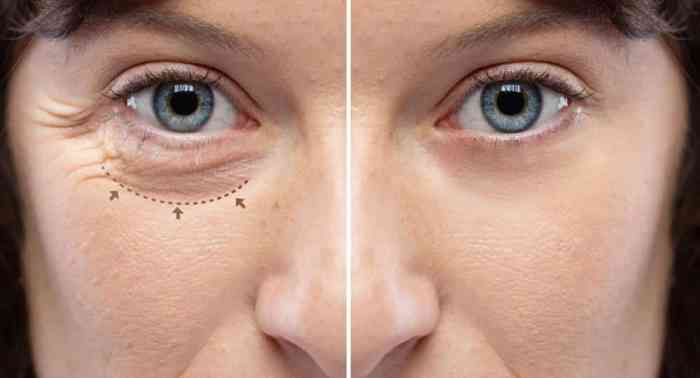
Insurance coverage for oculoplastic surgery, like any medical procedure, isn’t a simple yes or no. Several factors play a crucial role in determining whether your plan will cover the costs. Understanding these factors empowers you to navigate the process effectively.Oculoplastic surgery, focusing on the eye area, can involve a wide range of procedures, from treating eyelid abnormalities to correcting orbital issues.
Insurance companies assess the necessity and appropriateness of these interventions, often demanding pre-authorization. This meticulous review process safeguards against unnecessary procedures and ensures the patient receives the most appropriate care.
Factors Influencing Coverage Decisions
Insurance companies consider several key factors when evaluating oculoplastic surgery claims. These factors help determine the appropriateness of the procedure and its necessity in the patient’s treatment plan. Severity of the condition, extent of the proposed surgery, and the potential long-term benefits are assessed meticulously.
- Medical Necessity: The most crucial factor. Insurance companies need compelling evidence that the surgery is essential for addressing a specific medical problem. This includes a detailed diagnosis, supporting medical records, and a clear explanation of how the surgery will improve the patient’s condition. A detailed clinical report, including imaging and lab results, is critical for demonstrating medical necessity.
- Pre-authorization and Pre-approval Processes: Many insurance plans require pre-authorization or pre-approval before surgery. This step allows the insurer to review the proposed procedure, ensuring it aligns with their coverage guidelines and that it is medically necessary. A timely and comprehensive pre-authorization submission, including all relevant medical records and supporting documentation, is crucial.
- Patient’s Specific Health Insurance Plan: Different insurance plans have varying coverage policies. Some plans may cover a broader range of oculoplastic procedures than others. Understanding your specific plan’s details is paramount. Reviewing your policy documents or contacting your insurance provider directly will provide crucial information on specific procedures and their coverage.
- Severity and Complexity of the Condition: The severity and complexity of the eye condition directly impact the decision on coverage. More complex procedures, requiring specialized expertise and extensive time, may have different coverage requirements compared to less complex interventions. The complexity and duration of the proposed surgery are considered alongside the patient’s overall health.
Common Reasons for Claim Denials
Several reasons contribute to insurance claim denials for oculoplastic surgery. Understanding these common issues can help patients anticipate potential problems and prepare the necessary documentation to address them proactively.
- Lack of Medical Necessity: This is the most frequent cause. Insufficient documentation or a lack of evidence demonstrating the surgical intervention’s necessity can result in claim denials. The insurance company needs convincing evidence that the surgery is essential to the patient’s treatment plan and will provide significant benefits.
- Inadequate Pre-authorization or Pre-approval: Failure to complete the pre-authorization or pre-approval process correctly and on time can result in claim denials. Ensuring that all the required information is provided and submitted in a timely manner is essential for avoiding delays or rejection.
- Cosmetic Considerations: Surgery performed primarily for cosmetic reasons may not be covered. Insurance companies typically prioritize procedures addressing medical conditions, not aesthetic enhancements.
Illustrative Insurance Policies
This table provides a simplified overview of typical insurance policies regarding oculoplastic surgery, but it’s crucial to remember that specific coverage can vary significantly. Consult your insurance provider for detailed information.
| Insurance Company | Typical Policy |
|---|---|
| Company A | Generally covers medically necessary procedures, but requires pre-authorization. |
| Company B | May cover certain oculoplastic surgeries but may have exclusions for cosmetic procedures. |
| Company C | Typically covers procedures for conditions like ptosis, but may have limitations on complex procedures. |
Common Insurance Coverage Scenarios for Oculoplastic Surgery
Insurance coverage for oculoplastic surgery varies widely, depending on individual policies and the specific procedure. Understanding the nuances of coverage is crucial for patients to anticipate costs and plan accordingly. Factors such as pre-existing conditions, the extent of the procedure, and the surgeon’s credentials can all influence coverage decisions.
Typical Oculoplastic Procedures and Coverage Likelihood
Oculoplastic procedures often fall into categories, impacting the likelihood of insurance coverage. For example, procedures related to eyelid issues, such as blepharoplasty (eyelid lift) or ptosis repair (droopy eyelid correction), often have higher chances of coverage, particularly if medically necessary. Conversely, cosmetic procedures like brow lifts or aesthetic enhancements of the eye area may have less coverage or be entirely excluded.
- Medically Necessary Procedures: Procedures like ptosis repair, orbital decompression, and reconstructive surgery following trauma are typically more likely to be covered if deemed medically necessary by the insurance provider. The rationale is often based on restoring function or addressing a medical condition. Examples include treating tumors, correcting injuries, or restoring vision.
- Cosmetic Procedures: Blepharoplasty performed for cosmetic reasons alone usually has a lower chance of full coverage. Insurance companies often consider the aesthetic benefits to be less crucial than functional restoration. However, if a component of the surgery addresses a medical issue like excess skin interfering with vision, it might be considered a medically necessary element.
- Trauma-Related Procedures: Surgery resulting from accidents or injuries often has a higher likelihood of coverage, particularly if the procedure aims to restore function. Insurance companies recognize the medical necessity in these cases.
Circumstances Favoring Coverage
Insurance coverage is more likely when the oculoplastic procedure is medically necessary. A pre-operative evaluation from a qualified ophthalmologist or oculoplastic surgeon documenting the medical necessity and outlining the procedure’s rationale is vital. A clear diagnosis and documentation supporting the surgical intervention significantly enhance the chances of coverage.
Circumstances Less Likely to Receive Coverage
Cosmetic procedures are generally less likely to receive full coverage. The aesthetic enhancements are not viewed as critical medical necessities, and thus insurance companies often limit or deny coverage entirely. Insurance providers often use guidelines to distinguish between cosmetic and medically necessary procedures. It is advisable to thoroughly review the insurance policy for specific exclusions or limitations.
Verifying Coverage with Insurance Companies
Contacting the insurance company directly to clarify coverage for specific procedures is crucial. Be prepared to provide details about the procedure, including its medical necessity and rationale. Inquire about pre-authorization requirements, co-pays, and deductibles. Reviewing the Summary of Benefits and Coverage (SBC) document for the policy will also provide essential information. Using the insurance company’s online portal, if available, can speed up the verification process.
Examples of Successful Appeals
Successful appeals often involve compelling documentation. Cases where the surgeon documented the medical necessity and the procedure’s benefits in restoring function or addressing a medical condition are more likely to succeed. If a procedure is initially denied, a detailed appeal letter with supporting medical documentation can improve the chances of a favorable outcome. This often involves a strong explanation of the procedure’s purpose beyond cosmetic enhancements and its direct relation to the patient’s overall health.
Insurance Coverage Table Example
| Procedure | Likely Coverage (Medically Necessary) | Likely Coverage (Cosmetic) | Potential Out-of-Pocket Expenses |
|---|---|---|---|
| Ptosis Repair | High | Low | Co-pay, deductible |
| Blepharoplasty (Medically Necessary) | Moderate | Low | Co-pay, deductible, potential co-insurance |
| Blepharoplasty (Cosmetic) | Low | Very Low | Full out-of-pocket cost |
| Orbital Decompression | High | N/A | Co-pay, deductible, potential co-insurance |
Pre-Procedure Steps and Documentation
Oculoplastic surgery, while often crucial for eye health and function, necessitates careful pre-authorization and documentation to ensure smooth insurance claim processing. Understanding these steps is vital for patients and physicians alike, mitigating potential delays and ensuring timely access to care.Pre-authorization and pre-approval procedures are critical for navigating insurance complexities. This involves a proactive approach by both the patient and the surgeon, streamlining the process and minimizing potential roadblocks.
Accurate documentation is equally important, acting as a crucial link in the chain of ensuring successful claim resolution.
Pre-Authorization and Pre-Approval Procedures
Insurance companies often require pre-authorization or pre-approval for oculoplastic procedures. This involves submitting specific information to the insurance provider in advance of the surgery. The information required will vary based on the specific insurance plan and the nature of the procedure. The physician will initiate this process, often incorporating the patient’s specific needs and medical history. This early communication is essential for timely approval.
Necessary Documentation for Insurance Claims
Thorough documentation is critical for a successful insurance claim. This includes detailed medical records, physician notes, and imaging reports. Each element of the documentation provides critical information about the patient’s condition, the rationale for the surgery, and the expected outcome. The documentation is pivotal in justifying the necessity and appropriateness of the procedure.
Physician Communication with Insurance Companies
Effective communication between the physician and the insurance company is paramount. Physicians must clearly articulate the medical necessity of the oculoplastic surgery, using precise and compelling language to justify the procedure. This communication ensures that the insurance company fully understands the patient’s condition and the planned surgical intervention. Transparent communication can also help prevent delays and potential denials.
Typical Timeframe for Processing Insurance Claims
The timeframe for processing insurance claims can vary significantly depending on the complexity of the case and the specific insurance company. Some claims might be processed within a few weeks, while others might take longer. Factors such as pre-authorization requirements and the volume of claims processed can impact the timeframe. A proactive approach by the physician and the patient’s understanding of the process are key to expediting the claim.
Appealing Denied Claims
If an insurance claim is denied, the physician can initiate an appeal process. This process typically involves providing additional documentation and addressing any concerns raised by the insurance company. The appeal process requires a meticulous review of the denial reasons and a clear and concise response, providing further supporting evidence. This process often requires patience and persistence.
Documentation Required for Insurance Claims
| Category | Specific Documentation |
|---|---|
| Patient Medical Records | Complete medical history, including prior surgeries, diagnoses, and relevant imaging |
| Physician Notes | Detailed surgical plan, rationale for the procedure, and anticipated outcomes |
| Imaging Reports | CT scans, MRIs, or other relevant imaging studies supporting the surgical indication |
| Pre-authorization/Pre-approval Documents | Submitted forms and supporting correspondence with the insurance company |
| Surgical Consent Forms | Signed consent forms from the patient and, if applicable, the patient’s legal representative |
Potential Costs and Out-of-Pocket Expenses

Oculoplastic surgery, while crucial for eye health and function, can involve significant costs. Understanding these expenses upfront is essential for patients to make informed decisions about their care. Knowing potential out-of-pocket expenses empowers patients to plan financially and avoid surprises.Oculoplastic procedures can vary greatly in complexity and required resources. The estimated costs are influenced by the specific procedure, the surgeon’s fees, facility charges, anesthesia, and any necessary follow-up care.
Pre-operative evaluations, consultations, and post-operative appointments are additional factors.
Potential Costs Associated with Oculoplastic Surgery
Oculoplastic surgery encompasses a wide range of procedures, each with its own cost implications. Factors such as the surgeon’s experience, the complexity of the procedure, and the use of specialized equipment influence the overall cost. Procedures like eyelid surgery, orbital reconstruction, or lacrimal duct surgery all have unique price points.
Wondering if oculoplastic surgery is covered by insurance? It’s a crucial question for anyone considering the procedure. Navigating insurance can be tricky, but understanding your options is key. To get the best info, research your specific policy and potentially speak with a licensed insurance agent in Virginia, which can be helpful in understanding the complexities. Knowing how to become a licensed insurance agent in Virginia here could be a great way to learn more about navigating the process.
Ultimately, knowing your coverage details is essential for making informed decisions about your healthcare needs.
Common Out-of-Pocket Expenses
Beyond the surgical fee, patients often face additional costs. These may include pre-operative consultations, anesthesia fees, hospital or clinic facility charges, medications, and post-operative follow-up visits. The necessity for specific tests or imaging before surgery may also contribute to out-of-pocket costs.
Different Payment Options
Numerous payment options are available to patients to manage the financial burden of oculoplastic surgery. Insurance coverage is a key factor, but patients should explore options such as financing plans, payment plans, or patient assistance programs that may be available. Some surgeons or clinics might also offer flexible payment options.
Importance of Understanding Patient Financial Responsibility
Understanding your financial responsibility is crucial. Reviewing your insurance policy’s coverage details and any applicable deductibles, co-pays, and co-insurance amounts is paramount. Knowing your financial responsibilities will enable you to budget and make informed decisions about your treatment. Consult your insurance provider for clarification on your specific coverage.
Estimating Total Costs
Estimating total costs involves several steps. First, obtain detailed estimates from the surgeon or clinic about the surgical procedure, anesthesia, and facility charges. Second, consider potential out-of-pocket expenses like medications and follow-up care. Finally, confirm your insurance coverage to understand your portion of the cost.
Table Illustrating Potential Costs for Different Oculoplastic Procedures, Is oculoplastic surgery covered by insurance
“Accurate cost estimates depend on various factors, including location, surgeon’s experience, and the specific procedure.”
| Procedure | Estimated Surgery Cost (USD) | Estimated Out-of-Pocket Expenses (USD) | Notes |
|---|---|---|---|
| Blepharoplasty (Eyelid Surgery) | 2,500 – 5,000 | 500 – 1,500 | Can vary depending on complexity and surgeon’s fees. |
| Orbital Reconstruction | 6,000 – 15,000 | 1,000 – 3,000 | More complex, potentially involving multiple procedures. |
| Lacrimal Duct Surgery | 1,500 – 3,500 | 200 – 800 | Relatively less complex than other procedures. |
Resources for Patients

Navigating insurance coverage for oculoplastic surgery can be complex. This section provides crucial resources to empower patients in understanding their options and rights. Armed with this information, you can make informed decisions throughout the process.
Insurance Coverage Information Resources
Knowing where to look for insurance coverage details is key. Numerous resources can assist patients in this endeavor. Online portals of insurance companies often hold valuable information about coverage policies. Additionally, patient advocates and specialized websites offer insights and support.
- Insurance Company Portals: Direct access to your insurer’s website is often the first step. Look for a section on “coverage,” “benefits,” or “medical policies.” Specific policy details about oculoplastic procedures may be listed.
- Patient Advocacy Groups: Organizations like the American Academy of Ophthalmology or the National Eye Institute can offer valuable resources and support groups for patients facing similar situations. These groups may provide general information on coverage or direct you to relevant contacts.
- Specialized Oculoplastic Websites: Websites dedicated to oculoplastic surgery may offer insight into typical insurance coverage experiences, aiding in realistic expectations.
Insurance Claim Status Check
Checking the status of your insurance claim is important for understanding potential delays or issues. Most insurance companies have online portals for claim tracking. Reviewing the claim status regularly can help identify potential problems early on.
- Online Claim Tracking: Many insurers provide online portals for checking claim statuses. Access these portals through your insurer’s website, usually under a section like “Claims,” “My Account,” or “Manage My Claims.”
- Contacting Insurance Customer Service: Phone numbers for insurance customer service are readily available on your insurance policy documents or on the insurer’s website. Be prepared to provide claim details and policy numbers to expedite the process.
Cost Estimation Calculators
Online calculators can estimate the potential cost of oculoplastic surgery, including out-of-pocket expenses. These calculators consider factors like the specific procedure, location, and your insurance coverage details.
- Online Calculators: Several websites offer cost estimation calculators for medical procedures. These calculators can be valuable tools for budgeting and planning. Examples include tools from medical billing services or those provided by insurance companies.
- Professional Consultation: For a precise estimate, consult with your oculoplastic surgeon’s office or billing department. They can provide a detailed breakdown of anticipated costs, including potential out-of-pocket expenses based on your insurance.
Importance of Patient-Physician Communication
Open communication with your oculoplastic surgeon is crucial in discussing insurance-related concerns. This includes discussing potential out-of-pocket costs, insurance coverage details, and expected payment methods.
- Open Dialogue: Discuss your insurance plan with your oculoplastic surgeon. This will facilitate a clearer understanding of your potential financial responsibilities. Be sure to obtain detailed explanations of any anticipated out-of-pocket expenses.
- Clarify Coverage Gaps: Communicate any gaps or uncertainties in your insurance coverage with your surgeon. They can offer guidance on the best course of action to minimize financial burdens.
Contact Information
This table provides contact information for common insurance companies and relevant patient advocacy groups. Use this as a starting point for your research.
| Organization | Contact Information |
|---|---|
| [Insert Insurance Company 1] | [Insert Phone Number/Website] |
| [Insert Insurance Company 2] | [Insert Phone Number/Website] |
| [Insert Patient Advocacy Group 1] | [Insert Phone Number/Website] |
| [Insert Patient Advocacy Group 2] | [Insert Phone Number/Website] |
Wrap-Up
In conclusion, determining oculoplastic surgery coverage depends heavily on your individual insurance plan and the specific procedure. Understanding the pre-authorization process, required documentation, and potential costs is crucial. This guide has provided a comprehensive overview, highlighting key factors and steps to take to ensure a smooth and informed process. Remember, open communication with your physician and insurance provider is essential to clarify your coverage and any potential out-of-pocket expenses.
Commonly Asked Questions: Is Oculoplastic Surgery Covered By Insurance
Does my specific health insurance plan affect coverage for oculoplastic surgery?
Yes, your specific health insurance plan, including its network of providers and coverage limits, directly impacts the extent of oculoplastic surgery coverage. Different plans have varying policies on these types of procedures.
What documentation is typically needed for insurance claims related to oculoplastic surgery?
Medical records, physician notes, pre-authorization forms, and any necessary imaging results are usually required. Always check with your specific insurance company for the precise requirements.
How long does it typically take to process an insurance claim for oculoplastic surgery?
Processing times can vary considerably, depending on the insurance company and the complexity of the case. It’s wise to anticipate potential delays and keep an open line of communication with the insurance provider.
What are some common reasons for denial of claims related to oculoplastic surgery?
Common reasons for denial include missing pre-authorization forms, incorrect coding of the procedure, or lack of necessary medical documentation. Always review the denial notice thoroughly for specific reasons.



